2022.07.02.34
Files > Volume 7 > Vol 7 No 2 2022
1 Universidad Central del Ecuador – Instituto Superior de Posgrado, Quito-Ecuador
2 Unidad de Terapia Intensiva – Hospital Pablo Arturo Suárez, Quito-Ecuadorrge
Corresponding author Jorge Luis Vélez Páez E.mail [email protected]
Available from: http://dx.doi.org/10.21931/RB/2022.07.02.34
ABSTRACT
Encephalitis is a severe neurological syndrome with a rapid progression to encephalopathy caused by brain swelling. One of its causes is antibodies against neuron surface proteins, ionic channels, or receptors so that they can start encephalitis with psychiatric symptoms. Worldwide, auto-immune encephalitis annual incidence is 12.6 per 100000 inhabitants. We present a case report of a 44-years-old female who developed behavioral changes and seizures in a time-lapse of months. She was diagnosed with anti-GABA auto-immune encephalitis, a rare type of this disease.
Keywords. Auto-immune disease – Epilepsy – Mental disorders – Neurology – Critical Care
INTRODUCTION
Encephalitis is a severe neurological syndrome with a rapid progression to encephalopathy caused by brain swelling. It is characterized by fever, neurological focality, new-onset seizures, and electroencephalography (EEG) changes 1. Infectious diseases are one of its main etiologies; nevertheless, antibodies against neuron surface proteins, ionic channels, or receptors can start encephalitis with psychiatric symptoms 2.
Worldwide, auto-immune encephalitis is present more frequently in young people, with a peak at 21 years 3. The annual incidence is 12.6 per 100000 inhabitants. Anti N-methyl-D-aspartate receptor (NMDA) auto-immune encephalitis is the most common presentation; however, lack of identification of antibody happens in 40-50% of cases 2.
Early diagnosis and treatment are associated with a good prognosis. Initial immunotherapy has good results in the short and long term2.
A case report of a female patient of 44 years is presented, who developed behavioral changes and seizures in a time-lapse of months. She was diagnosed with anti-GABA auto-immune encephalitis, a rare type of this disease.
Case report
Forty-four-year-old female patient with a familiar history of schizophrenia presented to the emergency room with behavioral disorders and headache, without fever, parrhesia, or speech problems, is referred to Psychiatry because of suspicion of schizophrenia. Nevertheless, she developed generalized seizures upon her arrival and is hospitalized in Internal Medicine with a probable diagnosis of encephalitis. She is started on phenytoin, and antibiotics are indicated to cover a possible neuro-infection. Meropenem, vancomycin and fluconazole are used. Head and thorax computed tomography were indicated and resulted in normal.
The patient presented other seizures episodes. It was decided to administrate midazolam to control them and protect the airway, so she was put on mechanical ventilation and transferred to Intensive Care. Acyclovir is added to treatment in case of a possible viral infection. A lumbar punction was performed, and its results were expected (table 1). An electroencephalogram was carried out, and it showed it lateralized epileptiform cortical discharges in the right frontal lobule that spread to ipsilateral and contralateral regions.
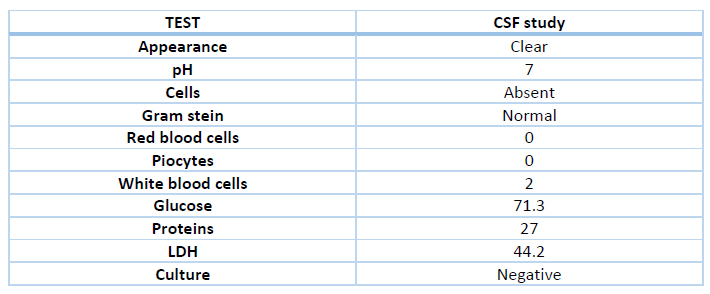
Table 1.- Cerebrospinal fluid test characteristics of the patient
Auto-immune encephalitis was considered in this clinical picture, and a sample of cerebrospinal fluid was sent to molecular studies. Methylprednisolone was indicated, and treatment allocation procedures were started. Immunoglobulins and plasmapheresis were considered first-choice treatments, even though they are not routinely available in the care facility where she was hospitalized.
The cerebrospinal fluid molecular studies returned and showed auto-antibodies anti GABARB1/B2.
Finally, after seven days of care, a vacant was available to move the patient and administrate an appropriate treatment. The patient was transferred on mechanical ventilation and sedatives. Phenytoin and lamotrigine were used as anticonvulsants. Antibiotics were stopped as no infectious diseases were active. Steroids were administered for five days and tapered accordingly.
DISCUSSION
It is presented the case of a young female who was initially diagnosed with schizophrenia and treated consequently. Nonetheless, she developed status epilepticus and needed sedatives and intensive care management. Auto-immune encephalitis was suspected, and an investigation for autoantibodies started. Anti GABA was positive, and treatment was allocated subsequently.
Ecuador does not have a formal registry for auto-immune encephalitis. Worldwide is reported an incidence of 12,6 cases per 100 000 inhabitants4, and 20% to 30% of these cases are related to autoimmunity5. It is described anti-NMDA auto-immune encephalitis as the most common variant2, and anti-leucine-rich glioma-inactivated 1 (LGI1) is the second in frequency with an incidence of 0.83 cases per 1 000 000 inhabitants6. Latin America neither has an incidence database about this pathology; however, several cases are reported, and published literature reviews show experience with this disease7, 8, 9.
High clinical suspicion is needed to accomplish diagnosis because non-specific symptoms are present like behavioral changes and seizures1. In our case, antibodies investigation was motivated by variability in the clinical picture, and anti-GABA resulted in positive.
There are two types of antibodies directed against the central nervous system: 1) antibodies against intracellular antigens (Hu type, Ri type, anti-fisine type, Ma2 type, CRMP 5-8-9-10) related to paraneoplastic syndrome with a poor response to treatment and a bad prognosis. 2) antibodies against surface and synaptic proteins (anti-AMPA-GluR3, anti-NMDA-NR1, anti-NMDA-NR2) better respond to first-line treatments10.
Anti GABA auto-immune encephalitis has an incidence of less than 5%11 of all cases. It happens more frequently in young female patients with refractory status epilepticus, behavioral changes, and severe psychiatric symptoms presentation1, 11. As depicted in our case report.
To accomplish diagnosis, a cerebrospinal fluid (CSF) study is imperative. It is described with: pleocytosis (>4/ul) in 69% of cases, proteins >0.5 g/l in 44% of cases, CSF to serum glucose ratio <0.5 in 27% of cases12. Our patient result was similar.
Literature reports show anti-GABA auto-immune encephalitis as strongly related to small cells lung cancer as in 50% of cases2, 4, 11; despite that, there is usually no clear trigger for this type of encephalitis1. Image thoracic studies in our patients do not display significant alterations.
In image studies, brain magnetic resonance image (MRI) usually shows changes in the hippocampus and amygdala in FLAIR and T2 sequences, cortical changes in FLAIR sequence and even a normal study2, 11. Our patient had a normal brain MRI.
Steroids are considered first-line therapy in anti-GABA auto-immune encephalitis cases, and plasmapheresis as second-line therapy1; 33% of patients have total remission to treatment and 40% with partial response4. When an oncologic cause is detected, treatment starts with antineoplastic therapy.
It has been reported that between 50% and 70% of auto-immune encephalitis cases require intensive care management and 41% mechanical ventilation. Intensive care length of stay has a mean of 89 days3. In our case, it was not possible to determine the total extension of hospitalization because the patient was transferred.
Despite a long hospital stay, recovery is encouraging; nevertheless, bad prognosis signs are central hypoventilation, movement disorder, abnormal MRI, late treatment, and lack of response to initial treatment13,14. Titulaer, et al3 reported that early treatment and non-intensive care unit (ICU) admission are related to good prognosis (OR 0.62, CI 0.50–0.76; p<0.0001; OR 0.12, CI 0.06–0.22; p<0.0001).
Limitations of this case were difficult to diagnose by identifying antibodies because this type of test is not common in Ecuador; our hospital is a second-level care facility, so there was a limitation to delivering appropriate treatment, and the patient needed transfer and follow-up was lost.
The strength of this report was high suspicion for auto-immune diagnosis after failure to initial antibiotic treatment, taking into account psychiatric subacute symptoms.
CONCLUSIONS
Auto-immune encephalitis is a rare disease with a low worldwide prevalence, so it is necessary to maintain a high clinical suspicion to achieve prompt diagnosis and treatment. Patient prognosis is related to it and avoiding the need for mechanical ventilation and ICU admission. Steroids are first-line drugs in these cases, with a third of patients having a good initial response, so plasmapheresis availability is key to continuing appropriate care. Patients can recuperate most of their functionality despite long recovery inside the hospital, and outpatient follow-up is essential for physiotherapy and reevaluation.
REFERENCES
1: Sonneville, R., Venkatesan, A. & Honnorat, J. Understanding auto-immune encephalitis in the ICU. Intensive Care Med 45, 1795–1798 (2019). https://doi.org/10.1007/s00134-019-05773-0
2: Ropper, Allan H.; Dalmau, Josep; Graus, Francesc (2018). Antibody-Mediated Encephalitis. New England Journal of Medicine, 378(9),840–851. doi:10.1056/NEJMra1708712
3: Titulaer MJ, McCracken L, Gabilondo I, Armangué T, Glaser C, Iizuka T, et al. Treatment and prognostic factors for long-term outcome in patients with anti-NMDA receptor encephalitis: an observational cohort study. Lancet Neurol. 2013 Feb;12(2):157–65
4: Diaz-Arias, L. A., Pardo, C. A., & Probasco, J. C. (2019). Autoimmune Encephalitis in the Intensive Care Unit. Neurointensive Care Unit: Clinical Practice and Organization, 249–263. https://doi.org/10.1007/978-3-030-36548-6_17
5: Granerod J, Ambrose HE, Davies NW, Clewley JP, Walsh AL, Morgan D, et al. Causes of encephalitis and differences in their clinical presentations in England: a multicentre, population-based prospective study. Lancet Infect Dis. 2010;10(12):835–44.
6: van Sonderen A, Petit-Pedrol M, Dalmau J, Titulaer MJ. The value of LGI1, Caspr2 and voltage-gated potassium channel antibodies in encephalitis. Nat Rev Neurol 2017;13:290-301.
7: Torres-Ballesteros Viviana, Murcia-Rojas Diana, Ochoa-Urrea Manuela, Vargas-Osorio Juliana, Bernal-Pacheco Oscar, Moreno Moreno Josué. Las diferentes facetas de la encefalitis autoinmune. Acta Neurol Colomb. [Internet]. 2020 Mar [cited 2021 Apr 29] ; 36( 1 ): 39-46. Available from: http://www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0120-87482020000100039&lng=en. https://doi.org/10.22379/24224022276.
8: Collao-Parra Juan Pablo, Romero-Urra César, Delgado-Derio Carolina. Encefalitis autoinmunes: criterios diagnósticos y pautas terapéuticas. Rev. méd. Chile [Internet]. 2018 Mar [citado 2021 Abr 29] ; 146( 3 ): 351-361. Disponible en: http://www.scielo.cl/scielo.php?script=sci_arttext&pid=S0034-98872018000300351&lng=es. http://dx.doi.org/10.4067/s0034-98872018000300351.
9: Mariño Nathalie, Triana Javier, Nieto Víctor, Vergara Jean Paul, Silva Miguel, Palacios Eduardo. ENCEFALITIS AUTOINMUNE: EXPERIENCIA DE UNA SERIE DE CASOS, Repertorio de Medicina y Cirugía, Mon, 25 Feb 2019. Disponible en https://revistas.fucsalud.edu.co/index.php/repertorio/article/view/876/925#info
Doi: DOI10.31260/RepertMedCir.v28.n1.2019.876
10: Torricelli RE. ENCEFALITIS AUTOINMUNES. RECEPTOR ANTI-NMDA Y NUEVOS INMUNOFENOTIPOS. 2019;6.
11: Höftberger R, Titulaer MJ, Sabater L, Dome B, Rózsás A, Hegedus B, Hoda MA, Laszlo V, Ankersmit HJ, Harms L, Boyero S, de Felipe A, Saiz A, Dalmau J, Graus F. Encephalitis and GABAB receptor antibodies: novel findings in a new case series of 20 patients. Neurology. 2013 Oct 22;81(17):1500-6. doi: 10.1212/WNL.0b013e3182a9585f. Epub 2013 Sep 25. PMID: 24068784; PMCID: PMC3888170.
12: Gable MS, Sheriff H, Dalmau J, Tilley DH, Glaser CA. The Frequency of Autoimmune N-MethylD-Aspartate Receptor Encephalitis Surpasses That of Individual Viral Etiologies in Young Individuals Enrolled in the California Encephalitis Project. Clin Infect Dis. 2012 Apr 1;54(7):899– 904.
13: Balu R, McCracken L, Lancaster E et al (2019) A score that predicts 1 year functional status in patients with anti-NMDA receptor encephalitis. Neurology 92:e244–e252. https ://doi.org/10.1212/WNL.00000 00000 00678 3
14: de Montmollin E, Demeret S, Brulé N et al (2017) Anti-N-methyl-d-aspartate receptor encephalitis in adult patients requiring intensive care. Am J Respir Crit Care Med 195:491–499. https ://doi.org/10.1164/rccm.201603-0507O C
Received: 21 June 2021 / Accepted: 25 February 2022 / Published:15 May 2022
Citation: Llerena-Rengel P, Rueda-Barragán F, Vélez-Páez J L. AntI GABA auto-immune encephalitis as schizophrenia and status epilepticus in a female patient: A case report. Revis Bionatura 2022;7(2) 34. http://dx.doi.org/10.21931/RB/2022.07.02.34
