2022.07.03.34
Files > Volume 7 > Vol 7 No 3 2022
Use of neural networks for triage of SARS-CoV-2
Jose Isaac Zablah1,*, Antonio Garcia Loureiro2, Salvador Diaz1, Yolly Molina1, Ana Cardona1, Jorge Urmeneta1, Ethel Flores1, Selvin Reyes Garcia1, Carlos A. Agudelo1, and Marco Tulio Medina1
1 Faculty of Medical Sciences, National Autonomous University of Honduras (UNAH); [email protected], [email protected], [email protected], [email protected], [email protected], [email protected], [email protected], [email protected], [email protected]
2 Department of Electronic and Computing, University Santiago de Compostela, Spain; [email protected]* Correspondence: [email protected]; Tel.: (504) 2239-4292
Available from: http://dx.doi.org/10.21931/RB/2022.07.03.34
ABSTRACT
Emergency services worldwide have been exceeded in their capacities due to the SARS-CoV-2 pandemic, a generalized situation in countries with robust health systems and aggravated in lagging countries. As a result, focused computer solutions have been developed for self-diagnosis, triage, and follow-up of suspected and confirmed patients of SARS-CoV-2. But as it is a new disease, the symptoms evolve in a short time and the diagnostic protocols must be updated. The applications that integrate algorithms in their code to help sanitary processes need to be modified, recompiled, and published integrating these changes. This article presents a solution through the implementation of a neural network that only requires updating an external file without the need to modify whole applications.
Keywords: SARS-CoV-2; Neural Network; Triage; Telemedicine; Cloud; Public Health
INTRODUCTION
In December 2019, the novel SARS-CoV-2 coronavirus was identified as the cause of the COVID-19 pandemic.1 Early symptom overlaps with other conditions such as the common cold and influenza, making early detection and diagnosis crucial for healthcare professionals. This is an acute respiratory tract disease whose management protocols are continuously evolving because it is caused by an unknown virus. It is difficult for medical personnel to keep up to date with management protocols, and the difficulty is even more significant when faced with the saturation of health care centers and, in addition to this, the overwork, which generates a high level of complexity in the treatment of patients.2-3
Nowadays, cloud-based technologies and the broad access to services based on the Infrastructure as a Service (IaaS) paradigm is the norm, generating a tendency to virtualize services with computational capacity in the form of Virtual Machines (VM), using elastic power in terms of resources in the deployment of IT solutions; allowing to deliver and distribute to many users in a short time multiple software solutions for specific purposes.4 These technologies were leveraged by the National Autonomous University of Honduras (UNAH) to develop a protocol for managing suspected and confirmed SARS-CoV-2 patients, which was subsequently integrated into a Doctor application 1847, which is currently available in Android and iOS-based device stores. This application is intended for use by the public and healthcare personnel at different levels.
The difficulty of software solutions-oriented to be used in the diagnosis of SARS-CoV-2 infection is that typically the patient evaluation forms need to be updated very often, which implies modifying the applications on mobile devices. This is laborious for developers and users who do not have broadband access to mobile or fixed Internet, a common situation in the Latin American region. In many countries, the digital divide resists closing, while in others, it is increasing, complicating the deployment of applications that need to operate offline without the possibility of frequent updates.5
To provide a helpful solution with the ability to combine the growing facilities of the cloud with a focus on changing protocols and the difficulty of broadband access, a neural network has been devised. These are defined as a series of algorithms that strive to recognize the underlying relationships in a set of data through a process that mimics the way the human brain works. In this sense, neural networks refer to systems of neurons, whether organic or artificial.
This article aims to show the benefits of using technologies related to neural networks in healthcare processes when testing an application during a pandemic emergency. Highlighting the ability of neural solutions to adapt to change faster than a human being. This article presents the organization of the source code, its logic and integration, and the details of its development so that it can be used by developers working to integrate management protocols into software solutions.
MATERIALS AND METHODS
The entire world has faced an unprecedented crisis due to the COVID pandemic. Multiple institutions have made the necessary resources available to deal with the health emergency and fully recover regular activity to face the changes caused by the pandemic. One of the main challenges in this regard is to stop the chains of contagion that may arise once mobility has been recovered and work, educational and commercial activity is reactivated. Artificial intelligence and neural networks have been used in various ways in software solutions to support the treatment of SARS-CoV-2. When writing, the most widely used use is for biomedical image analysis. Its applications have been grouped as follows:
· Digital tracking: They are based on techniques that use some form of passive or active surveillance. One of the studies presents the development of a method to guide people to protect themselves from someone who has high exposure to the virus or has symptoms of SARS-CoV-2. For this, different models of deep convolutional neural networks have been implemented by using an intelligent monitoring system (using cameras with certain specific capabilities), which become a complementary tool to be installed in different places so that people can automatically adopt biosecurity guidelines.6
Also, there is research related to the development of methodologies to predict the evolution over time of the number of individuals infected with SARS-CoV-2 in a country. Specifically, one is based on the synergy of explicit mathematical formulas and deep learning networks, which produce algorithms whose input is only the existing data in the country through the cumulative number of individuals reported to be infected. The analytical formulas involve several constant parameters, which were determined from the available data using an error minimization algorithm.
· Biomedical imaging: In one study, the use of models based on previously trained convolutional neural networks has been proposed for the detection of pneumonia in coronavirus-infected patients using thorax tomography, using three different binary classifications with four classes (COVID-19, normal (healthy), viral pneumonia and bacterial pneumonia). By using cross-validation, the performance results provided a very accurate classification of the patients, higher than 96% of efficiency.7
On the other hand, another article makes use of logistic regression with the before mentioned convolutional neural networks; this model uses a public repository of X-ray images of various patients. The results obtained for sensitivity and accuracy exceed 92% of efficiency.8
· Clinical data: These use medical data to diagnose, usually using some protocol. An article published by Banerjee 9 describes the use of machine learning in conjunction with simple statistical tests to identify SARS-CoV-2 positive patients using data from complete blood counts, but without knowledge of the individual's symptoms or medical history.
Another article is based on the fact that data analysis using machine learning accelerates optimized solutions in clinical healthcare systems. These essentially offer the efficient predictive capability and are a diagnostic alternative. Due to the prevalence of the spread of COVID-19, an urgent need has arisen in the healthcare industry to find a new drug to suppress the pandemic outbreak. A deep neural network model is presented that accurately considers the protein-ligand interactions of different medications. The response of protein-ligand interactions is detected to find the exchange that effectively fights the SARS-CoV-2 virus; this study uses the genomic sequences of patients that have been submitted to the GISAID database.10
The algorithm developed is from the group of solutions that operates with clinical data since it is intended to automate triage and can be integrated into any application that requires making decisions based on data. The tools used to develop the source code and training data of the decision tree of the neural network are described next. Notepad++ v7.8.5 editor was used for coding 11 and Python v3.7 programming language.12 The development libraries were as follows:
· TensorFlow: is a free, open-source software library for data flow and differentiable programming in various tasks. It is a symbolic mathematical library and is also used for machine learning applications such as neural networks, uses Apache 2.0 license, and is under the auspices of Google Research.13-15
· NumPy: is a library for the Python programming language, which adds support for arrays and multidimensional arrays, along with a collection of high-level mathematical functions for operating on these arrays. NumPy's ancestor, Numeric, was created by Jim Hugunin with contributions from several other developers and is offered under the BSD license.16-18
· Pandas: It is a software library for the Python programming language for data manipulation and analysis; it offers data structures and operations to manipulate numerical tables and time series. It supports importing data from various file formats such as comma-separated-values, JSON, and SQL, among others. Data manipulations that can be performed include merging, reshaping, selecting, as well as cleaning functions. It is released under the BSD license.19-21
The general methodology has been used to encode the algorithm.22 For the development of the neural network, there was a questionnaire made up of binary questions with a series of symptoms where each affirmative answer has a weight or score so that the most severe conditions increase an index that serves as a value that triggers the actions to be taken by the patient or health personnel. The structure of this questionnaire and its handling is detailed in Figure 1. The baseline questionnaire was developed by the Universidad Latina de Costa Rica by the COVID-19 Prevention Commission23 based on the guidelines of the Department of Health of Philippines,24 expanded by internists from the Facultad de Ciencias Medicas25 and Secretaria de Salud de Honduras,26 according to clinical experience.
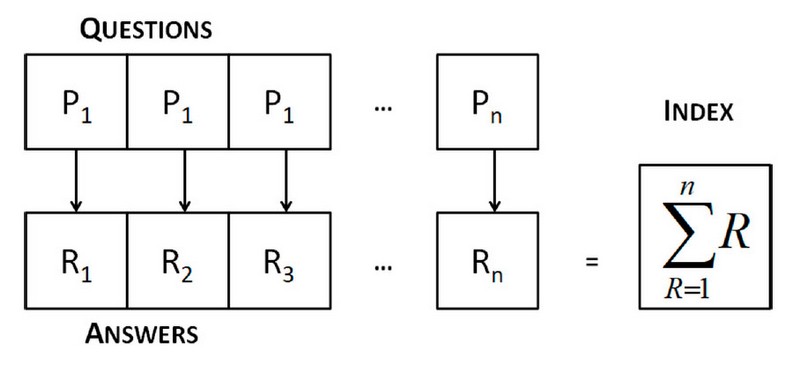
Figure 1. The questionnaire structure, the number of questions, and answers are expected to be altered as SARS-CoV-2 management protocols evolve.
For the training of the neural network, a comma-separated file was used with the answers to the different questions and their resulting index (sample and known data) so that each line represents a training element. The questions used on this occasion and their weights are described in Table 1, it is very likely that as the knowledge of SARS-CoV-2 infection expands, the questions are shown as well as the associated weights will vary. This file should be in the same folder where the source code is located.
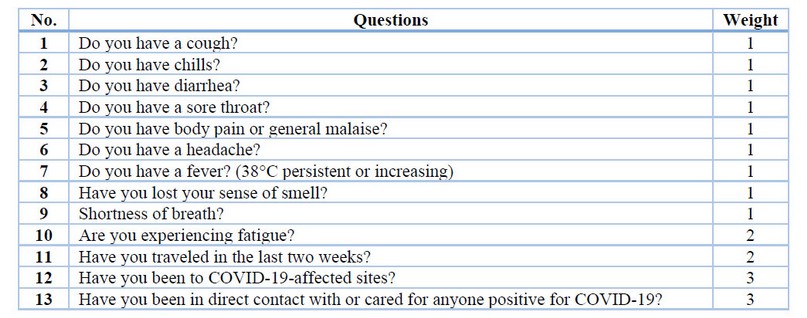
Table 1. Questionnaire for triage of the patient suspected of SARS-CoV-2 infection.
To train the neural network, the source code is executed with the interpreter, which will start the training process. The user can adjust the internal parameters of the program in terms of execution values according to his needs, considering that a neural network is a mathematical function that takes one variable and returns another, where both are considered vectors. The structure of a simple neural network is shown in Figure 2.
The connections between each neuron have a weight-adjusted by an iterative training process. Generally, there is a layer of weights between the input and output called the hidden layer. Additionally, the hyperparameters are variables that are defined before the training of the neural network; the way the network will be trained is defined by the number of hidden layers and the learning rate, while the structure is determined by the learning rate (which takes values from 0 to 1) and the decay gradient that is linked to a defined optimization function.
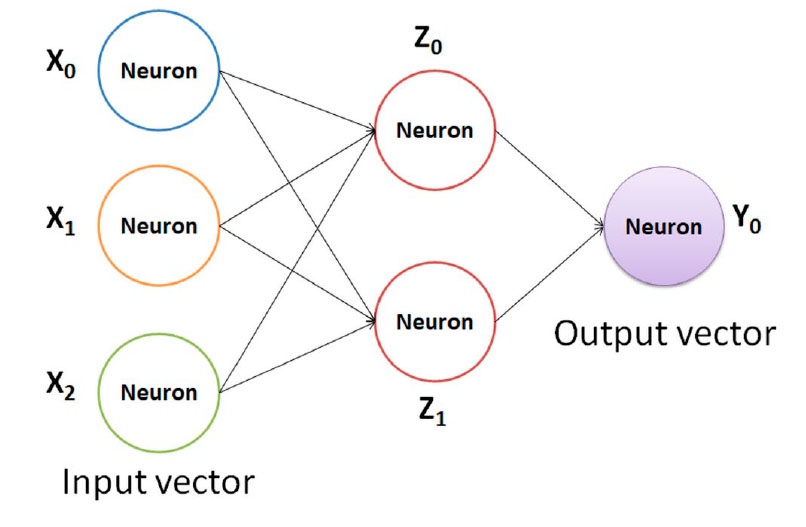
Figure 2. Structure of a basic neural network. The arrows indicate the connection of neurons.
The learning rate is the speed at which the model learns, which is linked to additional parameters that serve to refine the error distribution; this helps to update the weights of the connections between neurons each time the training is executed. Depending on the optimization algorithm, a decay of the learning rate may occur, varying during exercise; in other cases, it remains constant in each of the epochs (or training iterations). The important thing is to achieve that the learning rate has convergent values; this is the property of finite functions to get closer and closer to a limit when a variable of a function varies in terms of a series; this gives rise to the existence of the decay, to adjust the weights dynamically during training.
The neural network proposed in this paper uses the Adam (Adaptive moment optimization) optimizer,27 this algorithm implements a method that calculates individual adaptive learning rates for different parameters from estimates of the first and second moments of the gradients. This optimizer was chosen because it is simple to implement, is computationally efficient, has low memory requirements, and is suitable for problems that are large in terms of data. It is also ideal for non-stationary situations and issues with very noisy or sparse gradients.
Upon completion of the neural network training, several resulting files are obtained, which are described in Table 2. These files contain the variables, operations, network design and parameter values. The purpose of these files is to continue the evolution of the network by having a more significant number of data and parameters, including the possibility of implementing the training in a production application.
To evaluate the validity of our algorithm, different mathematical methods will be used. In the field of artificial intelligence and especially in the problem of statistical classification, a confusion matrix is a tool that allows visualizing the performance of an algorithm used in supervised learning. The benefit of a confusion matrix is to make it easy to see if the system is confusing classes.28 The ROC (Receiver Operator Characteristic) curve is a graph used to show the diagnostic capabilities of binary classifiers. It was first used in signal detection theory but is now used in many other areas such as medicine, radiology, natural hazards, and machine learning.
It is constructed by plotting the actual positive rate (TPR) against the false positive rate (FPR). The true positive rate is the proportion of observations that were correctly predicted as positive out of all positive observations, known as true positive (TP) and false negative (FN) derived from (TP / (TP + FN)). Similarly, the false positive rate is the proportion of observations that are incorrectly predicted as positive out of all negative comments as known as false positive (FP) and true negative (TN) derived from (FP / (TN + FP)). For example, in medical tests, the actual positive rate is the rate at which people are correctly identified to test positive for the disease in question.29
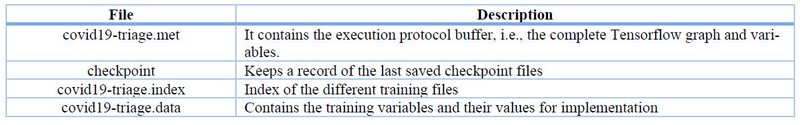

Table 2. Files resulting from the neural network training.
RESULTS
The results are presented as a comparison of the staff's diagnoses against what was obtained by the algorithm. This is to make evident the advantages of both diagnostic mechanisms.
Confusion Matrix
To verify that the classification algorithm has a performance that allows it to be used with sufficient confidence to aid in the triage of SARS-CoV-2 suspects, a tool is known as a confusion matrix was used.22 This is a technique for summarizing the performance of a classification algorithm; by calculating it, you can get a better idea of what is doing well and what types of errors are being made. It is important to note that the classification accuracy variable alone can be misleading if you have an unequal number of observations in each class.
By performing clinical auscultation based on the experience and memory of healthcare personnel in triage, taking a sample of 3256 people, of which 2241 were classified as not having the disease (true negatives (TN)), 670 were positive at the clinical level but were classified as negative (false negatives (FN)), 339 identified as positive (true positives (TP)) and of these 6 were negative at the clinical level but were erroneously classified as positive (false positives (FP)). The true positives were confirmed with laboratory analysis.
The data above showed an actual positive rate of 0.983, which indicates the ability of the algorithm used to correctly detect the disease; this is known as sensitivity. The actual negative rate is 0.770, which describes the ability to accurately identify healthy patients, called specificity. The false-positive rate is 0.230, and the false-negative rate is 0.017. The accuracy of this classification is 0.792. The specificity of this classification was 0.770.
By using the questionnaire together with the neural network, we proceeded to implement it to take a sample of 128 people independent to avoid data bias. They used the implementation of this neural network on a mobile application called Doctor 1847,30. They were followed up for a month and a half until they had a valid clinical test to confirm the pathology under study. Of these samples, 44 people did not have the disease, and the algorithm classified them as negative (true negative), six were positive at the clinical level, and the algorithm classified them as negative (false negative), and 76 coincided as positive between test and algorithm (true positive) and two were negative at the clinical level, but the algorithm classified them as positive (false positive).
Type I errors are equivalent to 7.68%, and Type II has a proportion of 3.84%; these values are low and result from good class balancing. This, together with the sensitivity of the questionnaire and the efficient design of the neural network algorithm, offers a viable solution for triage. Using the confusion matrix, the neural network showed a precision of 0.927, an accuracy of 0.938, a true positive rate of 0.974 (sensitivity), and the true negative rate is 0.880 (specificity). The false-positive rate is 0.120, and the false-negative rate is 0.026. The specificity of this classification was 0.880. Compared with the results of human triage, the use of the neural network has a better behavior.
ROC Curve
The ROC curve in our case shows the balance between sensitivity (or TPR) and specificity (1-FPR). Classifiers that give curves closer to the upper left corner indicate better performance. As a baseline, a Random classifier is expected to score points along the diagonal (FPR = TPR). The closer the curve is to the 45-degree diagonal of the ROC space, the less accurate the test will be. Note that the ROC does not depend on the class distribution. This makes it useful for evaluating classifiers that predict rare events such as disease or disaster. In contrast, assessing performance using precision (TP + TN) / (TP + TN + FN + FP) would favor classifiers that always predict a negative result for rare events.
To compare different classifiers, it may be helpful to summarize the performance of each classifier in a single measure. A common approach is to calculate the area under the ROC curve, which is abbreviated as AUC. It is equivalent to the probability that a randomly chosen positive instance will rank higher than a randomly chosen negative. A classifier with a high AUC may occasionally score worse in a specific region than another classifier with a lower AUC. But in practice, the AUC works well as a general measure of predictive accuracy. In Figure 3, you can see the behavior of the classification, with a better score of neural networks. In these results, the total sample, 3256 people, is considered. To these data, the neural network was applied and compared with the results of human triage.
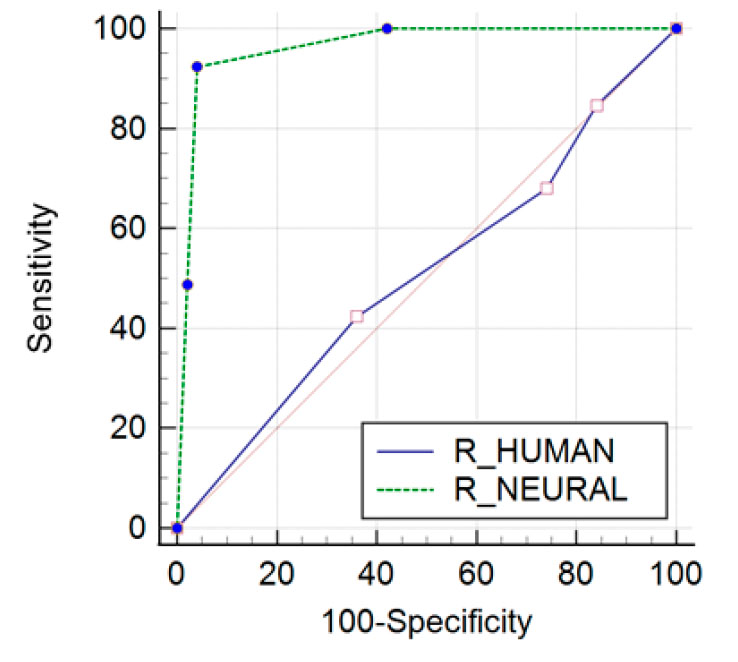
Figure 3. The sensitivity of the neural network R_NEURAL is higher than the human R_HUMAN. Care in triage using only the experience of health professionals was at the minimum acceptable.
The area under the curve (AUC) and standard error (SE) and confidence interval (CI) with better values using neural network (R_NEURAL); when comparing the statistics of both classification algorithms, their differences are marked since the sensitivity and specificity of the neural network exceed human capabilities. It is shown in Table 3 that there is a difference in the area under the curve of 0.455, and this value is supported by a standard error of 0.0545, indicating a low variance between the sample of each of the algorithms. The confidence interval is in the upper middle region of the AUC, with a minimum level of significance that invalidates a null hypothesis. SE was obtained using the DeLong method.31
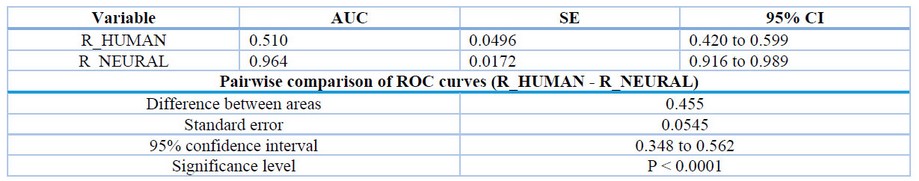
Table 3. Ranking stats comparison.
The samples used have high sensitivity, but as far as accuracy is concerned, the classification of triage using health experience is very low (0.336) compared to that shown by the neural network (0.927); the same can be said for specificity, which was higher for the neural network than for human triage. As for the false negative rate, the neural network performed a worse classification than its counterpart, but as for the false positive rate, it was better than the human classification.
DISCUSSION
It is necessary to be aware that the results on this occasion greatly benefit triage using neural networks. Still, we must not neglect that the nature of the human being is more effective when needing action in unusual or exceptional moments. Hence, technology is only a tool to accelerate results. Neural networks cannot create knowledge; they can decide autonomously based on training based on previous events that sensitize them according to the different methods and applications for which they have been designed. The proposed neural network behaves with the same efficiency as others published for similar purposes, with high levels of sensitivity and specificity, making them very reliable for sanitary purposes.
The neural network represents a technical advantage in the medium and long term. However, initially, it is not sufficiently sensitive to the heuristic results presented; it can save technical hours in crises, as it can only be trained with base data. The results obtained make it a viable solution in complex applications and situations of high variability, but at no time does it replace the experience and common sense of a health professional. However, as technology evolves, it may be achieved. Humans will most likely surpass technology in detecting exceptions and new situations for several years.
Changes in needs cause care protocols to be modified and health personnel to be trained; this is a slow, lengthy, and costly task. The use of technologies makes it possible to close this gap for the benefit of patients since it would give time to update what is necessary. This process can be dangerous because if the expert who gives the guidelines is wrong in expressing them or has flaws, it can cause a solution to generate cascading problems, complicating care and distorting the advantages of adopting technology.
On a large scale, if artificial intelligence is developed with criteria of quality and relevance to be used for health purposes, it can be expected to obtain speed and more excellent coverage of health services. Still, there will always be a margin of situations in which a human professional should intervene. And many ethical criteria should evolve and adapt since the results shown in this work show that humans have a behavior that can be improved technologically.
CONCLUSIONS
Since the revolution of informatics and computer technology in the 1980s, mankind has become increasingly involved with technology in various areas of knowledge. Health sciences are currently receiving a great deal of attention and development. The emergence of new pandemic threats occurs spontaneously; unlike in the past, now we have more tools and knowledge to face them.
SARS-CoV-2 is a disease caused by a coronavirus, which has wreaked havoc on many people, as well as on the economic and productive levels of countries. Mortality reaches 5% of infected patients in specific geographic regions, but the recovery and after-effects of suffering from this disease require months to be fully overcome. The decrease in the quality of life of infected, recovered, and healthy patients is notorious due to social restrictions, which force society, in general, to make use of technology for production and health purposes.
The use of neural networks offers advantages as a valuable tool to adapt to complex variable situations; in this study, the developed algorithm classified COVID-19 patients much better than health personnel, mainly due to presenting a consistent behavior over time; instead, the human depends on many other factors. While the staff cannot be removed, combining a more robust technology can significantly benefit the patient.
Science benefits from technology because it allows it to accelerate processes, model and take better quality data. The neural network proposed here demonstrates the flexibility required in situations of high variability, where human capacity is exceeded by the high volume of data to be analyzed. The use of hard coding or a stored questionnaire, updated in databases and applications, requires the modification of software and data structures in servers for later distribution in the terminal equipment, with the consequences of implementation and debugging in each version. On the other hand, a neural network can be ported into an application and updated online, allowing the use of heterogeneous multi-origin data and not limited to closed-response questionnaires.
The data has high accuracy and sensitivity, which indicates that it has sufficient capacity to handle the different conditions of the users that employ a neural network implementation. Caution should be taken that incremental evolutions of the algorithm and questionnaire used as a source and data management do not present the phenomenon called imbalance (this is a highly accurate model but with a low sensitivity or specificity); in that case, it should be made to proceed to perform a class balancing. But the results obtained when analyzing the data through a confusion matrix and the ROC curve have shown that the neural network presented for triage tasks can be trusted.
The use of computerized systems in triage allows rapid adaptation to changes in treatment protocols for infectious diseases such as SARS-CoV-2 to maturity that would allow use for long periods without the need for changes in applications. This provides healthcare professionals with less reliance on their memory skills and would give them time to strengthen their clinical capabilities.
The use of artificial intelligence technology in primary care applications, specifically in triage and reduction of delays due to infections caused by the SARS-CoV-2 virus, is feasible and should incorporate follow-up data from laboratory studies and deep biomedical image analysis networks. The algorithm combined with the questionnaire provides a neural network with the capacity to be used in production for triage since high accuracy, sensitivity, and specificity are obtained that equals or exceeds that of humans.
Supplementary Materials: No
Author Contributions: Conceptualization, J.I Zablah and S. Diaz; methodology S.Diaz, J. Urmeneta, E. Flores; software J.I Zablah and A. Garcia-Loureiro, validation S. Reyes Garcia and M.T. Medina; formal analysis S. Diaz and A. Cardona; investigation J.I. Zablah and C. A. Agudelo; review Y. Molina. All authors have read and agreed to the published version of the manuscript.
Funding: No funding received.
Institutional Review Board Statement: Not applicable.
Informed Consent Statement: Not applicable.
Data Availability Statement: This study did not report any data.
Acknowledgments: We thank the Directorate of Humanistic and Technological Scientific Research (DICIHT) for the support provided for the publication of this manuscript.
Conflicts of Interest: The authors declare no conflict of interest.
REFERENCES
1. Kevadiya B.D., Machhi J., Herskovitz J. et al. Diagnostics for SARS-CoV-2 infections. Nat. Mater. 2021, 20, 593–605: doi: 10.1038/s41563-020-00906-z
2. Karim S. S. A. & Karim Q. A. Omicron SARS-CoV-2 variant: a new chapter in the COVID-19 pandemic. The Lancet, 2021, 398, 2126-2128. doi: 10.1016/S0140-6736(21)02758-6
3. Birje M. N., Challagidad P. S., Goudar R. H., & Tapale M. T. Cloud computing review: concepts, technology, challenges and security. Int. J. Cloud Computing, 2017, 6(1), 32-57.
4. TOMCZYK Łukasz, et al. Digital Divide in Latin America and Europe: Main characteristics in selected countries. In 14th Iberian Conference on Information Systems and Technologies (CISTI). IEEE, Coimbra, Portugal, 2019. 1-6. doi: 10.23919/CISTI.2019.8760821
5. Dölen M & Lorenz R. General Methodologies for Neural Network Programming. Int. j. smart eng. syst. des., 2002, 4, 63-73, doi:10.1080/10255810210629
6. A. Narin, C. Kaya, and Z. Pamuk. Automatic Detection of Coronavirus Disease (COVID-19) Using X-ray Images and Deep Convolutional Neural Networks. ArXiv Pre-prints. Available: http://arxiv.org/abs/2003.10849 (accessed on 10 March 2020).
7. M. I. Uddin, S. A. A. Shah, and M. A. Al-Khasawneh. A Novel Deep Convolutional Neural Network Model to Monitor People following Guidelines to Avoid COVID-19. J. Sens., 2020, 1–15. doi: 10.1155/2020/8856801
8. A. S. Fokas, N. Dikaios, and G. A. Kastis. Mathematical models and deep learning for predicting the number of individuals reported to be infected with SARS-CoV-2. J. R. Soc. Interface, 2020, 17, 169. doi: 10.1098/rsif.2020.0494
9. A. Banerjee, S. Ray, B. Vorselaars, J. Kitson, M. Mamalakis, S. Weeks, M. Baker, and L. S. Mackenzie. Use of Machine Learning and Artificial Intelligence to predict SARS-CoV-2 infection from Full Blood Counts in a population. Int. Immunopharmacol., 2020, 86, 106705. doi: 10.1016/j.intimp.2020.106705
10. N. Yuvaraj, D. K. Srihari, S. Chandragandhi, R. A. Raja, D. Dr. Gaurav, and K. Dr. Amandeep. Analysis of Protein-Ligand Interactions of SARS-CoV-2 against Selective Drug using Deep Neural Networks. Big data min. anal. 2021, 4, 76-83. doi: 10.26599/BDMA.2020.9020007
11. D. Ho and others. Notepad++. Available online: http://notepad-plus-plus. Org (Accessed on 20 January 2020)
12. T. E. Oliphant. Python for Scientific Computing. Comput Sci Eng, 2007, 9-3, 10–20. doi: 10.1109/MCSE.2007.58
13. M. Abadi, P. Barham, J. Chen, Z. Chen, A. Davis, J. Dean, M. Devin, S. Ghemawat, G. Irving, M. Isard. Tensorflow: A system for large-scale machine learning. In 12th Symposium on operating systems design and implementation, Savannah, USA, 2016, 265–283. Available online: https://www.usenix.org/conference/ osdi16/technical-sessions/presentation/abadi (Accessed on 3 March 2020)
14. TensorFlow. Available online: https://www.tensorflow.org/ (Accessed on 10 February 2020)
15. F. Ertam and G. Aydin. Data classification with deep learning using Tensorflow. In International Conference on Computer Science and Engineering (UBMK)-IEEE, Antalya, Turkey, 2017, 755–758. doi: 10.1109/UBMK.2017.8093521
16. NumPy: Numerical Library. Available online: https://numpy.org/ (Accessed on 1 April 2020)
17. S. van der Walt, S. C. Colbert, and G. Varoquaux. The NumPy Array: A Structure for Efficient Numerical Computation. Comput Sci Eng, 2011, 13-2, 22–30. doi: 10.1109/MCSE.2011.37
18. T. E. Oliphant. Object Essentials, In A guide to NumPy. Trelgol Publishing, USA, 2006; 1, 18-43
19. Pandas Library. Available online: https://pandas.pydata.org/ (Accessed on 1 April 2020)
20. W. McKinney. Pandas Powerful Python Data Analysis Toolkit, 2012. Available online: https://pandas.pydata.org/pandas-docs/version/0.7.3/pandas.pdf (Accessed on 31 July 2022)
21. Pandas, python data analysis library. Available online: http://pandas.pydata.org (Accessed on 1 April 2020)
22. Visa S, Ramsay B, Ralescu A, et al. Confusion matrix-based feature selection. MAICS, 2011, 710, 120-127.
23. Universidad Latina de Costa Rica. Available online: https://www.ulatina.ac.cr/ (Accessed 14 June 2020)
24. 2019-nCoV Interim Guidelines of Department of Health of Phillipines. Available online: https://www.doh.gov.ph/node/19217 (Accessed on 14 June 2020)
25. Facultad de Ciencias Médicas - UNAH. Available online: https://fcm.unah.edu.hn/ (Accessed on 31 July 2022)
26. Secretaria de Salud - Honduras. Available online: http://www.salud.gob.hn/site/ (Accessed on 31 July 2022)
27. D. P. Kingma and J. Ba. Adam: A Method for Stochastic Optimization. In 3rd International Conference for Learning Representations, San Diego, USA, 2014. doi: 10.48550/arXiv.1412.6980
28. F. Provost and R. Kohavi. Glossary of Terms. Mach Learn, 1998, 30-2, 271–274. doi:10.1023/A:1017181826899
29. Kamarudin A. N., Cox T. & Kolamunnage-Dona, R. Time-dependent ROC curve analysis in medical research: current methods and applications. BMC Med. Res. Methodol, 2017, 17, 1-19. doi: 10.1186/s12874-017-0332-6
30. Doctor 1847. Available online: https://doctor1847.unah.edu.hn/#/login (Accessed on 31 July 2022)
31. E. R. DeLong, D. M. DeLong, and D. L. Clarke-Pearson. Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics, 1988, 44, 837–45. doi: 10.2307/2531595
Received: 21 March 2022 / Accepted: 27 July 2022 / Published:15 August 2022
Citation: Zablah J I, Loureiro A G, Diaz S, Molina Y, Cardona A, Urmeneta J, Flores E, Reyes Garcia S, Agudelo C A, Medina M T. Use of neural networks for triage of SARS-CoV-2. Revis Bionatura 2022;7(3) 34. http://dx.doi.org/10.21931/RB/2022.07.03.34
