2022.07.02.36
Files > Volume 7 > Vol 7 No 2 2022
Sddiq Ghani Al-Muhanna 1*, Israa Abdul Ameer Al-Kraety 2 and Shaima Rabeea Banoon 3
1 Department of Anesthesia Techniques, Faculty of Medical and Health Techniques, University of Alkafeel, Najaf, Iraq; [email protected]
2 Department of Medical Laboratory Techniques, Faculty of Medical and Health Techniques, University of Alkafeel, Najaf, Iraq; [email protected]
2 Department of Biology, College of Science, University of Misan, Maysan, Iraq.; [email protected]
Available from: http://dx.doi.org/10.21931/RB/2022.07.02.36
ABSTRACT
A newly discovered coronavirus, COVID-19, creates a new infectious illness. According to current clinical observations, people's age and gender appear to have a role in their vulnerability to COVID-19. This research aims to see whether there is an association between gender, age, and COVID-19 susceptibility in the public health department of Najaf. The study included 36607 subjects (evenly distributed between sexes), and their ages ranged from (<10 - 80) years. According to the study's findings, males were found to be more infected than females. Results of the research indicated that gender and Covid-19 had a strong correlation. According to the study, people between the ages of 30 and 39 were more common than people of other ages range. The study's findings revealed a significant difference between Covid-19 and the participants' ages.
Keywords. Covid-19; Gender; Age; Najaf; Iraq.
INTRODUCTION
As part of the Nidovirales order, the Coronaviridae family, Coronaviruses, are classified. The term "coronavirus" refers to the virus's outer surface, which is covered with spikes that resemble a crown. Coronaviruses have genetic material consisting of a single-stranded RNA molecule ranging from 26 to 32 kilobases (kb). Coronaviruses are very tiny viruses (65-125 nm in diameter). Coronavirus family subgroups are alpha (α), beta (β), gamma (γ), and delta (δ) 1. Due to the COVID-19 epidemic, there has been an unparalleled level of crises in contemporary times 2. The severity of the disease varies greatly from person to person, ranging from moderate or even subclinical infection to full-blown disease 3 & 4.
More than 1 million COVID-19-related deaths have been recorded over the globe. There has been no viable treatment or vaccination for this infectious disease as of this writing. Several elements might affect the development of COVID-19; thus, it's essential to identify them. Potential risk factors for infection and illness progression are of interest. As a result of several medical and epidemiological studies, it has been concluded that all communities are in danger of infection. However, several risk factors have been linked to an increased incidence of COVID-19, and age may be one of these. Even though COVID-19 may affect persons of various ages, the elderly are the most vulnerable. Pediatric patients less than one year of age have been reported to have more severe clinical symptoms. COVID-19 may potentially put newborns at risk of respiratory failure, according to certain studies 5. The severity of the condition in males was shown to be higher than in females, suggesting that gender may be a risk factor for COVID-19. When it comes to COVID-19 infections, males are generally more susceptible to death than women 6, and the study's goal is to conduct a statistical analysis of conditions by gender and age.
MATERIALS AND METHODS
For coronavirus infection, data on age and gender were collected from the public health department and Najaf hospital in Najaf province in 2021. As a result, to evaluate the impacts, the Statistical Analysis System program (SPSS) was utilized. The Chi-squared test was used.
RESULTS AND DISCUSSION
The study revealed males (57%) were found to be more infected than females (43%), as shown in Figures (1); this result agrees with de Souza et al.,2020. COVID-19 causes a disproportionately high number of deaths in men, prompting the hypothesis that men are more at risk than women. Males are more likely to die from heart disease, diabetes, liver disease, and cancer than females 7. COVID-19's sex-biased mortality maybe because these illnesses have been shown to have a sex-specific incidence. Men in Italy die at a greater rate than men in China. It is assumed that the increased incidence of cardiovascular disease among Italian males is responsible, as an example 8. Males and females differ in their susceptibility to infection, ability to withstand stress, and total lifespan. In certain nations, females outlive their male counterparts by over seven years 9. According to Pradhan and Olsson's Biology of Sex Variations, sex-related differences, including variances in hormone composition, heredity, and other physiological features, may be to blame for this discrepancy in life expectancy. Evidence suggests that females may outlast their male counterparts even under the worst conditions, such as hunger 9. In Sweden, male life expectancy was slashed to 17.15 years during the 1772–1773 famine, while female life expectancy rose to 18.79 years. An estimated 18.7 and 22.4 years of life expectancy were slashed by the Irish famine of 1845–1849. Male life expectancy decreased from 41.58 years to 7.3 years, while female life expectancy decreased from 45.93 years to 10.9 years 9. Other historical instances suggest that men are less able to deal with challenging conditions than women in terms of their level of endurance. In the first year of their voyage back to Africa, 43 percent of the formerly enslaved Americans died. Male's life expectancy was 1.68 years, and females' was 2.23 years 9.
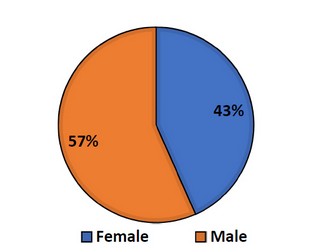
Figure 1. Rate of infection according to gender
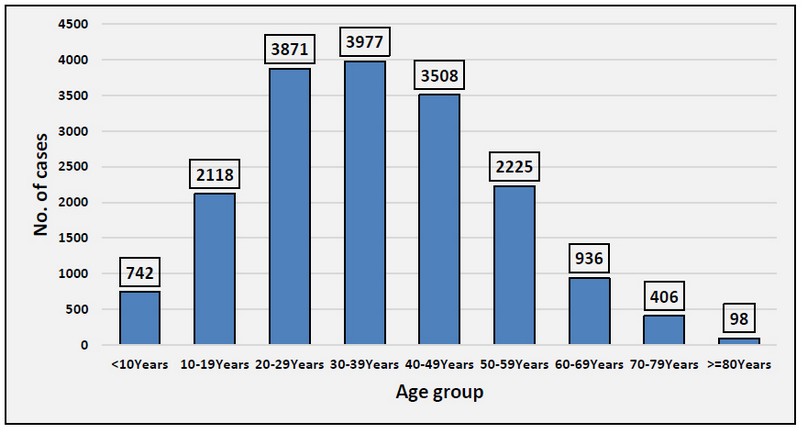
Figure 2. Distribution covid-19 infection according to age
As shown in Figure 2, those between the ages of 30 and 39 were older than those between the ages of 40 and 49; this finding aligns with 10. A personal encounter with COVID-19 between 18 and 69 may have helped them estimate their risk perception of the virus 11 & 12. Participants above the age of 70 did not use the heuristic to estimate the hazard presented by COVID-19 in the research, perhaps because of reduced cognitive resources. Among sociodemographic factors, only in the age range of 40–49 was being female associated with significant risk levels 13. Moreover, in the 30-39 age range, having a job predicted a greater chance of exposure. Subjective health perceptions were detrimental in explaining risk susceptibility in the ages of 18-29 and 50-59, respectively. People in these age groups may assume they are more susceptible to COVID-19 because they have poor physical health. As for emotions, tension-anxiety and hostility-anger indicated vulnerability in the age groups of 30-39 and 50-59. In younger people aged 30–39, higher levels of tension-anxiety were linked to a lower risk susceptibility. Be aware that this POMS subscale does not reflect COVID-19-specific anxiety levels but rather general levels of stress and anxiety in general. Aggressive-hostile adults in the 50–59 age bracket showed a decreased susceptibility 14.
CONCLUSIONS
The study revealed males were found to be more infected than females. The study also mentioned that infection with COVID-19 focused on 30 -39 years old.
Author Contributions: "Conceptualization, SGA and IAA; methodology, SGA and IAA; software, SRB; validation, SGA, IA.A and SRB; formal analysis, IAA; investigation, SGA; resources, S.GA.. and IAA; data curation, SGA, IA.A and SRB; writing—original draft preparation, IAA; writing—review and editing, SGA and SRB; visualization, IAA; supervision, SGA; project administration, IAA; funding acquisition, SGA, IA.A and SRB. The published version of the work has been reviewed and approved by all authors."
Funding: "There was no outside support for this study.".
Informed Consent Statement: Not applicable
Acknowledgments: The president of the University of Alkafeel is thanked by the authors for their assistance in completing this study.
Conflicts of Interest: "The writers have stated that they have no conflicts of interest to disclose.."
REFERENCES
1. Shereen MA, Khan S, Kazmi A, Bashir N, Siddique R. COVID-19 infection: Emergence, transmission, and characteristics of human coronaviruses. Journal of advanced research. 2020 Jul 1;24:91-8.
2. Saleh H, AL-KAHLIDI MU, Abulridha HA, Banoon SR, Abdelzaher MA. Current situation and future prospects for plastic waste in maysan governorate: effects and treatment during the COVID-19 pandemic. Egyptian Journal of Chemistry. 2021 Aug 1;64(8):4449-60.
3. Wiersinga WJ, Rhodes A, Cheng AC, Peacock SJ, Prescott HC. Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID-19): a review. Jama. 2020 Aug 25;324(8):782-93.
4. Isam JZ, Kamil KZ, Banoon Shaima R. Review about COVID-19. Research Journal of Biotechnology Vol. 2021 Apr;16(4):229-33
5. Ge H, Wang X, Yuan X, Xiao G, Wang C, Deng T, Yuan Q, Xiao X. The epidemiology and clinical information about COVID-19. European Journal of Clinical Microbiology & Infectious Diseases. 2020 Jun;39(6):1011-9.
6. Sharma G, Volgman AS, Michos ED. Sex differences in mortality from COVID-19 pandemic: are men vulnerable and women protected?. Case Reports. 2020 Jul 15;2(9):1407-10.
7. Heron MP. Deaths: leading causes for 2015. 2017.
8. Di Stadio A, Ricci G, Greco A, De Vincentiis M, Ralli M. Mortality rate and gender differences in COVID-19 patients dying in Italy: A comparison with other countries. Eur Rev Med Pharmacol Sci. 2020:4066-7.
9. Regan JC, Partridge L. Gender and longevity: why do men die earlier than women? Comparative and experimental evidence. Best practice & research Clinical endocrinology & metabolism. 2013 Aug 1;27(4):467-79.
10. Tversky A, Kahneman D. Availability: A heuristic for judging frequency and probability. Cognitive psychology. 1973 Sep 1;5(2):207-32.
11. Liu M, Zhang H, Huang H. Media exposure to COVID-19 information, risk perception, social and geographical proximity, and self-rated anxiety in China. BMC public health. 2020 Dec;20(1):1-8.
12. Guastafierro E, Toppo C, Magnani FG, Romano R, Facchini C, Campioni R, Brambilla E, Leonardi M. Older adults’ risk perception during the COVID-19 pandemic in lombardy region of italy: a cross-sectional survey. Journal of Gerontological Social Work. 2021 Aug 18;64(6):585-98.
13. Dryhurst S, Schneider CR, Kerr J, Freeman AL, Recchia G, Van Der Bles AM, Spiegelhalter D, Van Der Linden S. Risk perceptions of COVID-19 around the world. Journal of Risk Research. 2020 Aug 2;23(7-8):994-1006.
14. Lerner JS, Keltner D. Beyond valence: Toward a model of emotion-specific influences on judgement and choice. Cognition & emotion. 2000 Jul 1;14(4):473-93.
Received: 22 February 2021 / Accepted: 29 March 2022 / Published:15 May 2022
Citation: Al-Muhanna S, Ameer Al-Kraety I , Rabeea Banoon S. Statistical Analysis of COVID-19 infections according to the gender and age in Najaf Province, Iraq. Revis Bionatura 2022;7(2) 36. http://dx.doi.org/10.21931/RB/2022.07.02.36
